Doctor-Patient Relationship

“The doctor didn’t even look at me before writing out a prescription!”
“That patient’s relatives threatened me about the consequences if she doesn’t recover.”
“The doctor was very critical and judgmental about me.”
“That doctor cannot even guarantee that my wife will recover with his treatment!”
That’s not all. Ordering unnecessary tests, prescribing unnecessary and costly medicines, needless admission to hospital, performing unwarranted surgery, negligence in care, etc., are the usual accusations by patients. Having unrealistic expectations, assuming that doctors are always after money, not respecting the doctor’s time, etc., are how doctors frequently lament about patient attitudes.
The relationship between patients and doctors is shifting fast in the current times, driven by many factors in modern healthcare. This relationship is indispensable in the practice of medicine and it is critical to achieving reasonable clinical outcomes. We can enjoy a deep sense of satisfaction from a good doctor-patient relationship. But it can be a source of intense discomfort and harm to both doctors and patients when the relationship is strained.
The four cornerstones of any relationship are trust, respect, appreciation and time; they are very relevant to a doctor-patient relationship too.
However, in the current ‘fast’ world, these qualities are generally scarce. As a result, mistrust, allegations, lawsuits, and atrocities have resulted in many unfortunate situations.
Doctor-Patient Relationship in Ancient Times
However, such issues were not unheard of in ancient times too. The following two Sanskrit shlokas tell us a lot about the doctor-patient relationship in ancient times, though jokingly.
- वैद्यराज नमस्तुभ्यम् यमराज सहोदर ।
यमस्तु हरति प्राणान् वैद्यः प्राणान् धनानिच ॥
My salutations to you, oh doctor! You are the brother of Yamaraja (God of death). While Yama takes only our lives, you take our life and wealth too! - चिताम् प्रज्वलिताम् दृष्ट्वा वैद्यो विस्मयमागतः । नाहङ्गतो नमे भ्राता कस्यैदं हस्त लाघवम्? ॥
A doctor returning to his hometown is surprised to see a burning funeral pyre – “I was away as was my brother, then who else is responsible for this?”
Since time immemorial, the society has expected doctors to have competence, honesty, empathy, accountability and professionalism.
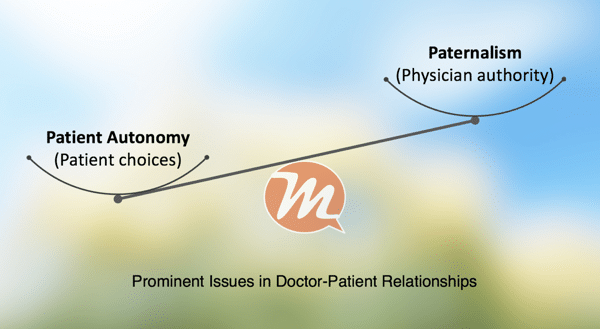
The Canterbury vs Spence case of 1972 opened a Pandora’s box of lawsuits and showed the legal risks of medical practice in the modern world. Since then, the discussion about the doctor-patient relationship has focused on the two extremes of autonomy and paternalism.
Models of Doctor-Patient Relationship
There are four models of doctor-patient relationship based on varying combinations of autonomy and paternalism.
- Paternalistic Model: Doctors use their skills to determine the patient’s diagnosis, stage of disease and the best mode of treatment. Then, they provide the patient with selected information that will encourage the patient to consent to the plan of treatment that the doctor considers best. In this model, the doctor acts as the patient’s guardian, doing what is best for the patient, in their opinion. Patient autonomy is limited to agreeing to the doctor’s advice. However, except in the rare situations of a medical emergency where the time taken to obtain an informed consent might harm the patient, this paternalistic model has no role in the current times.
- Informative Model: The doctor provides the patient with all relevant information so that the patient can select the intervention that he or she wants, and the doctor executes that option. In this model, the doctor is the source of information and technical expertise, and the patient has the total autonomy to choose the intervention that suits their values and affordability. This is an antithesis of the paternalistic model.
- Interpretive Model: The doctor understands the patient’s values, and helps the patient select the appropriate intervention that achieves what the patient wants. Here, usually, the patient is vague about their expectations, therefore, the doctor is a mentor, with an obligation to not only provide information but also to elicit and interpret patient expectations and values.
- Deliberative Model: The doctor provides information, understand patient values and helps the patient in deciding to choose the best treatment option in the given situation. Here, the patient is clear about their expectations and values, and therefore, the doctor is like a friend, involving the patient in a discussion on which course of action would be the best.

All the above models have varying degrees of patient autonomy. But there is another model called “instrumental model” where the patient has no freedom. Here, the patient values are irrelevant, and the doctor aims for a goal unrelated to the patient, like the good of society or advancement of scientific knowledge. While this model has undergone moral condemnation, it is still applicable in situations where the patient is a direct and intentional threat to public health.
The Best Model
Different models may be appropriate in different clinical circumstances. However, it is important to specify one model as the pragmatic reference; while we do not condemn other models automatically, they require justification based on the circumstances. An ideal relationship does not vest the entire decision-making to either the doctor or the patient alone; a process of shared decision making with mutual participation and respect is ideal.
Doctors bring their medical training, evidence-based knowledge and expertise to the diagnosis and management of their patients’ condition. Patients bring knowledge of their personal values and preferences. The benefits and risks of various options in the treatment can be evaluated through these patient values and preferences.
It is generally accepted that “deliberative model” is probably the best model to follow in routine clinical situations. Patients also need to be clear about their expectations and values for this model to work.
Evidence-based medicine (EBM), which is the foundation of modern medicine, is very relevant here and clearly sums this up too.
Evidence-Based Medicine
EBM is the conscientious, explicit, judicious and reasonable use of modern, best evidence in making decisions about the care of individual patients.
The focus on evidence does not exclude the role of patients. As depicted in the image below, EBM is an integration of the doctor’s clinical expertise, the patient’s values and relevant research evidence. An efficient application of EBM, with all these characteristics, is capable of delivering better and cost-effective healthcare.
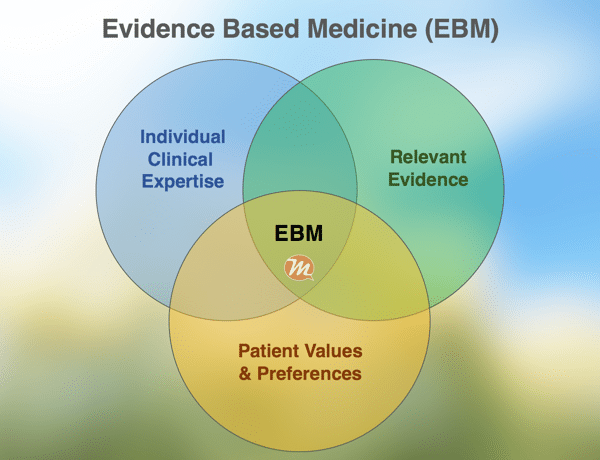
Clinical Decision Making
The essence of doctoring is a combination of knowledge, understanding, teaching and action. The caring doctor integrates the patients’ clinical condition and personal values and makes a recommendation on the appropriate course of action. The doctor also tries to educate the patient about the advantages, disadvantages and cost-benefits of this approach.
Clinical relationships require the same focus and attention as technical competence. It is no wonder that this is an extremely complex issue.
The purpose of a good doctor-patient relationship and evidence-based medicine is aptly summarised in this Sanskrit universal prayer:
सर्वे भवन्तु सुखिनः । सर्वे सन्तु निरामयाः।
सर्वे भद्राणि पश्यन्तु। मा कश्चित् दुःख भाग्भवेत्॥
May all be prosperous and happy, may all be free from illness,
May all appreciate what is spiritually enlightening, may no one suffer.
Further reading: New Dimensions in Patient-Physician Interaction








Doctor-patient Relationship: A well wriien wrieup…But to sum it up in short as a reader first, i agree that its foremost important especiallt when the world has become commercial n relationship values hve become materialistic.. Understanding two way communication between two individual gives best of results where i believ one is a listener n one is a sayer……
As a Patient, i would like to say that i have a very good doctor in you for both mom n me… I thank god for this…🙏
Thank you very much for your appreciation!